Physical Address
304 North Cardinal St.
Dorchester Center, MA 02124
Physical Address
304 North Cardinal St.
Dorchester Center, MA 02124
Sutik Biswasindian journalist
 British Broadcasting Corporation
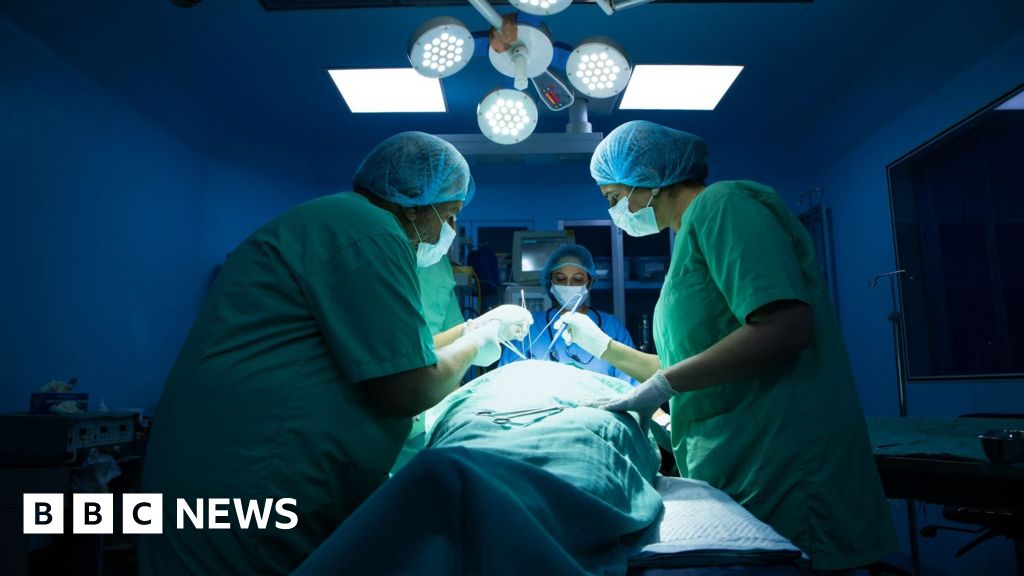
British Broadcasting CorporationUnder the harsh lights of an operating room in Delhi, India’s capital, a woman lay motionless as surgeons prepared to remove her gallbladder.
She was under general anesthesia: unconscious, unconscious, completely still with a cocktail of drugs that induced deep sleep, blocked memories, dulled pain and temporarily paralyzed her muscles.
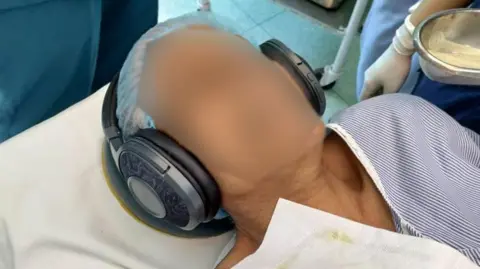
Yet, amid the hum of the monitors and the steady rhythm of the surgical team, soft flute music emanated from the headphones on her ears.
Although the drug quieted much of her brain, her auditory pathways remained partially active. When she wakes up, she regains consciousness faster and with greater clarity because she requires lower doses of anesthetic drugs, such as propofol and opioid painkillers, than patients who don’t hear the music.
At least, that’s New peer-reviewed research Advice from Maulana Azad Medical College, Delhi. The study, published in the journal Music & Medicine, provides the strongest evidence yet that music played during general anesthesia can modestly but meaningfully reduce the need for medication and improve recovery.
The study focused on patients who underwent laparoscopic cholecystectomy, the standard keyhole procedure to remove the gallbladder. The procedure is short—usually less than an hour—and requires particularly quick, “clear-headed” recovery.
To understand why researchers are turning to music, it helps to interpret modern anesthesia practice.
“The goal is to leave the hospital as early as possible after surgery,” said Dr. Farah Hussain, senior specialist in anesthesia and a certified music therapist on the study. “Patients need to wake up clear, alert, oriented, and ideally pain-free. With better pain management, the stress response will be reduced.”
Achieving this requires a carefully balanced combination of five or six medications that keep patients asleep, relieve pain, prevent surgical memory, and relax muscles.
 Getty Images
Getty ImagesDuring surgeries such as laparoscopic cholecystectomies, anesthesiologists now often supplement this drug regimen with local “blocks,” ultrasound-guided injections that numb nerves in the abdominal wall.
“General anesthesia plus block is the norm,” said lead researcher Dr. Tanvi Goel, former senior resident at Maulana Azad Medical College. “We’ve been doing this for decades.”
But the body does not readily accept surgery. Even under anesthesia, it reacts: heart rate rises, hormones surge, blood pressure spikes. Reducing and managing this cascade is one of the central goals of modern surgical care. Dr. Hussain explains that the stress response can slow recovery and worsen inflammation, underscoring why careful management is so important.
The stress begins even before the first cut, the insertion of a breathing tube into the trachea via intubation.
To do this, the anesthesiologist uses a laryngoscope to lift the tongue and soft tissue at the base of the throat, get a clear view of the vocal cords, and guide the tube into the trachea. This is a routine step under general anesthesia to keep the airway open and provide precise control of the patient’s breathing while they are unconscious.
“Laryngoscopy and intubation are considered to be the most stressful reactions during general anesthesia,” said Dr. Sonia Wadhawan, director and professor of anesthesia and critical care at Maulana Azad Medical College and director of the study.
“Even though patients are unconscious and don’t remember anything, their bodies still respond to stress with changes in heart rate, blood pressure and stress hormones.”
To be sure, medicine has evolved. The old etheric mask has disappeared. Instead, intravenous drugs—most notably propofol, a sleeping pill michael jackson dies But it is prized in the operating room for its quick onset of action and clean recovery. “Propofol takes effect in about 12 seconds,” Dr. Goel noted. “We prefer it for short-term surgeries such as laparoscopic cholecystectomy because it avoids the ‘hangover’ caused by inhaled gas.”
The research team wanted to know whether music could reduce patients’ need for propofol and fentanyl, an opioid painkiller. Less medication means faster awakening, more stable vital signs and fewer side effects.
So they designed a study. A pilot project involving eight patients followed a full 11-month trial in 56 adults aged approximately 20 to 45 years, randomized into two groups. All received the same five-drug regimen: drugs to prevent nausea and vomiting, sedatives, fentanyl, propofol and muscle relaxants. Both groups wore noise-canceling headphones, but only one group heard the music.
“We ask patients to choose from two calming instruments – a flute or a piano,” says Dr. Hussain. “There are still areas of the subconscious mind that remain active. Even if the music is not explicitly recalled, implicit awareness can have beneficial effects.”
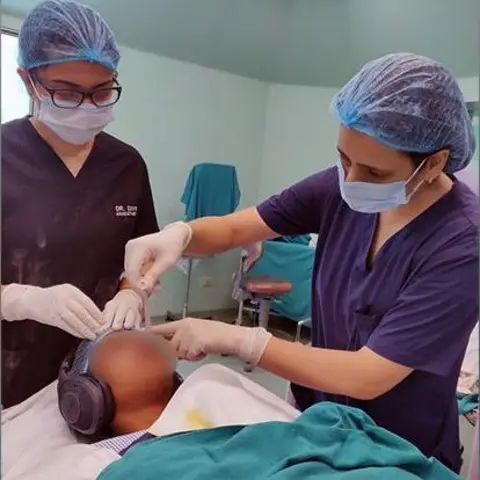
The results are stunning.
Patients exposed to music require lower doses of propofol and fentanyl. They experienced smoother recovery, lower cortisol, or stress hormone, levels and better blood pressure control during surgery. “Because auditory abilities remain intact under anesthesia, music can still shape the brain’s internal state,” the researchers wrote.
Apparently, music seems to calm the inner storm. “Even if you lose consciousness, the auditory pathways remain active,” Dr. Wadhavan said. “You may not remember the music, but the brain registers it.”
The idea that minds behind the veil of anesthesia are not entirely silent has long intrigued scientists. Rare case of ‘intraoperative awareness’ shows patient recalling snippets of operating room conversation.
If the brain is able to pick up and remember stressful experiences during surgery (even if the patient is unconscious), then it may be able to record positive or comforting experiences, such as music, even without conscious memory.
“We are just beginning to explore how the unconscious mind responds to non-pharmacological interventions such as music,” said Dr. Hussain. “It’s a way to humanize the operating room.”
Music therapy is not new to medicine. It has long been used in psychiatry, stroke rehabilitation and palliative care. But its move into the high-tech, machine-controlled world of anesthesia marks a quiet shift.
If such a simple intervention can reduce medication use and speed recovery—even modestly—it could reshape how hospitals think about surgical health.
As the team builds on their earlier findings and prepares for the next study exploring the effects of music-assisted sedation, one fact is already emerging from the data: Even when the body is still and the mind is asleep, a few soft notes appear to help kick-start recovery.